|
|
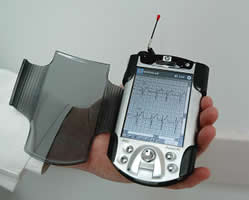
Paramedic’s EKG Transmits to Cardiologist’s Handheld Computer; Heart Attack Patient Goes from Scene Straight to Cath Lab New Digitized Heart Imaging Information System Sets New Emergency Heart Catheterization Benchmark at 33 Minutes from National Average 104 Minutes Concord, NC, October 2, 2003 - A new digitized Cardiac and Imaging Information System at NorthEast Medical Center that links Cabarrus County paramedics to cardiologists and emergency medicine teams at Northeast Medical Center has led to a national patient "door-to-dilation" record. "Door-to-dilation" response time includes the time between the patient’s arrival at a cardiac catheterization lab and the successful completion of an angioplasty procedure to alleviate the effects of a blocked coronary artery. The national average is 104 minutes. The process involves preparing the catheterization (cath) lab to receive the patient, assembling the procedure team, prepping the patient, locating the blockage and inserting a balloon device to reduce pain and symptoms—all hopefully before damage from lack of blood flow impacts the heart muscle. Following his exercising at a local gym, a 41-year old resident had chest pains. Upon arrival home, his daughter called the paramedics, who started their evaluation.
This early notification allows for assembly of the heart team prior to patient arrival, allowing direct transport to the cath lab. If paramedics have questions or problems, the emergency physician is always available by radio. The patient’s EKG transmission went straight to Paul Campbell, MD, cardiologist on call at the hospital. Dr. Campbell viewed the EKG reading transmitted from the patient’s home, and quickly determined he immediately needed a cardiac cath due to blockage of a coronary artery. Without quickly restoring proper blood flow to the heart muscle, the patient could experience heart damage or even death.
Prior to implementing the system, NorthEast’s median door-to-dilation time was 93 minutes, less than the national average of 104 minutes. But after implementing and connecting the new technology and procedures from the field to cath lab, that former time has been reduced by two-thirds. “Everything came together to make this happen with outstanding results for our first patient using the new system and protocols,” explains Dr. Campbell. “We hope this event can serve as an excellent example what can happen when technology, people and careful planning work together to save lives.”
|
||||||||||||||
© PDA cortex. All
Rights Reserved
IT's Cutting Edge