|
|
|
|
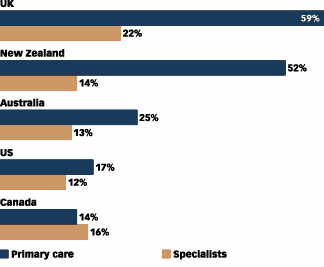
Canada & U.S. Trails Other Countries in Use of EMR and Electronic Prescribing
Many experts agree on two steps that could be taken to significantly improve the quality of care and to reduce medical errors. Both involve the use of information technology and electronic documentation. In both areas, North America is not moving nearly as fast as the experts would like. Indeed, the U.S. is moving more slowly than some other countries. One major reason for medical errors is that different physicians treating the same patient do not all have access to all the patient's medical records. Different, incomplete medical records are kept in different places. There is a near consensus that the widespread use of electronic medical records, accessible to all those seeing and treating a patient substantially improves the coordination and quality of care. Another important reason for medical errors is that most prescriptions are still written on paper, and mistakes are made in the filling of prescriptions because they are difficult to read or incomplete, or merely because of human error. Again there is a near consensus that electronic prescribing would greatly reduce prescribing errors, thereby improving the quality of care. For example, their use would avoid many of the problems caused by drug interactions, a cause of many hospital admissions. While almost every expert who has written or spoken on this subject agrees that the use of electronic prescribing and electronic medical records would greatly reduce medical errors, implementing these changes can be slow, difficult and expensive. In many cases there are no financial, or other, incentives to physicians or health systems to implement them. Research has shown that many physicians see no benefit to themselves or their practices by moving from paper to electronic systems. As a result, Harris Interactive research shows only relatively small minorities of American physicians are using electronic records or prescribing, and the United States lags behind other English speaking countries in this regard. A survey of physicians conducted for the Harvard School of Public Health and the Commonwealth Fund's International Health Care Symposium in 2000, found that the use of electronic systems is much more advanced in Britain, New Zealand and Australia than in the United States. The data for Canadian usage were also low, similar to those in the U.S. The biggest differences between countries, by far, were in the use of electronic systems by primary care physicians rather than by specialists. For example, the proportions of primary care physicians who were (sometimes) using electronic medical records were 17% in the U.S., 14% in Canada, 25% in Australia, 52% in New Zealand and 59% in the U.K.
And the proportions of primary care physicians who were using electronic prescribing "often" were 9% in the U.S., 8% in Canada, 44% in Australia, 52% in New Zealand and 87% in the U.K. Differences between Primary Care Physicians and Specialists The use of electronic medical records and electronic prescribing was lower (mostly far lower) among specialists than among primary care physicians, except in Canada where it was slightly higher. Here again, however, the U.S. lags the other countries, with the lowest proportions of specialists using either electronic medical records or prescribing. Why Is Usage Higher in Other Areas and Lower Here? There is a simple explanation for these differences in the US. In countries with national health services, or universal government-funded health insurance, there is a single payer (whether that is the federal or state, or provincial government). The single payer sets the rules. If the single payer says physicians must use electronic systems, they will do so. Furthermore, they can dictate a single nationwide system. However that explanation does not shed light on why Canada lags in the adotion of EMR. The U.S., has thousands of different employer-provided health plans, hundreds of insurers and managed care plans, and 50 state Medicaid systems. This pluralism makes it very much more complicated, more difficult and more expensive to introduce new electronic systems. It seems almost certain therefore that the U.S. will continue to trail far behind many other countries in the uses of information technology, in spite of the consensus that they would substantially reduce medical errors, improve the quality of care, and possibly save money.
|
|||||
© 2001 PDA cortex.
All Rights Reserved
IT's Cutting Edge